Treatment of Severe Destructive Foot and Ankle Injury in a Young Child with a Skin Regeneration Technique
By Xueping Luo1, Xiaoming Chen1, Guofeng Lei2Affiliations
doi: 10.29271/jcpsp.2022.06.833Sir,
Severe destructive foot and ankle injuries in children are most often caused by traffic accidents, crushing by heavy objects, and machine strangulation and are often combined with injuries to the skin, subcutaneous tissue, tendons, vessels, nerves, and bones, which require multiple surgical treatments.1 Some patients with severe injuries may experience toe necrosis and even permanent loss of the parts distal to the forefoot, midfoot, and ankle, resulting in various degrees of disability.2
In April 2018, a 3-year child with a severe destructive injury to the left foot was admitted to our hospital. Fracture reduction, internal fixation, and vascular and nerve repair surgery were performed in the Emergency Department (ED). On the second day, skin on the dorsum and toes 1-3 of her left foot gradually started to develop a dark purple appearance, and debridement and toe amputation were planned. On day three, physical examination revealed that the skin of the entire dorsum, sole, and medial side of the foot distal to the wound on the left ankle was bluish-purple, and some areas were blackish-purple with scattered blisters; the skin was bluish-purple at the base of toes 1-3 and blackish-purple at the tips of the toes (Figure 1).
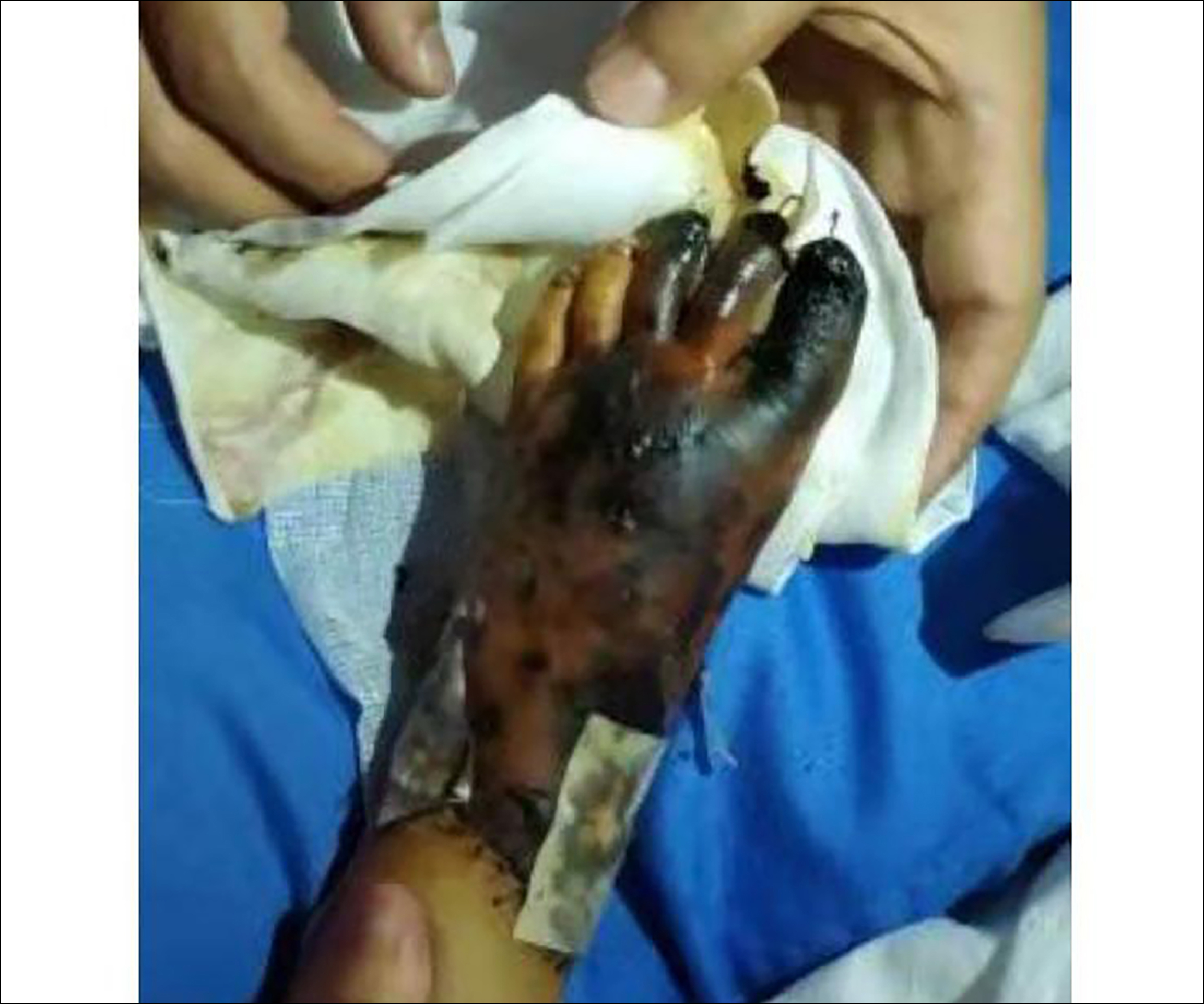 Figure 1: Three days after the injury, the skin of the dorsum distal to the left ankle was bluish-purple, and most of it was dark. The skin of toes 1-3 was blackish-purple in colour, without blood supply.
Figure 1: Three days after the injury, the skin of the dorsum distal to the left ankle was bluish-purple, and most of it was dark. The skin of toes 1-3 was blackish-purple in colour, without blood supply.
The patient was shifted to the Orthopedic Ward. After hospitalization, the patient received active anti-infection and symptomatic treatment, and her vital signs were stable. In-situ skin regeneration, moist exposed burn ointment (MEBO), wound, and ulcer dressing were planned. The skin on the dorsum of the left foot had high tension and obvious ecchymosis. A small incision was made to reduce the tension, and a rubber strip was placed for drainage. When the dressing was changed three days later, the wound, drainage exudate, and secretions were cleaned with normal saline. The dressing was changed once each day. Twelve days later, the necrotic areas of the skin of the dorsum and sole were limited, and the necrotic tissue surrounding the drainage port was reduced. Twenty-three days later, the black skin scabs gradually fell off, and fresh granulation tissue formed under the wound. By days 52 to 58, wounds on the dorsum and sole were completely epidermised. The distal phalanges of toes 1-3 of the left foot were absent, and the wounds on the stumps were healed. The child had a normal arch, a normal forefoot width, good limb movement, and no obvious contractual sequelae (Figure 2).
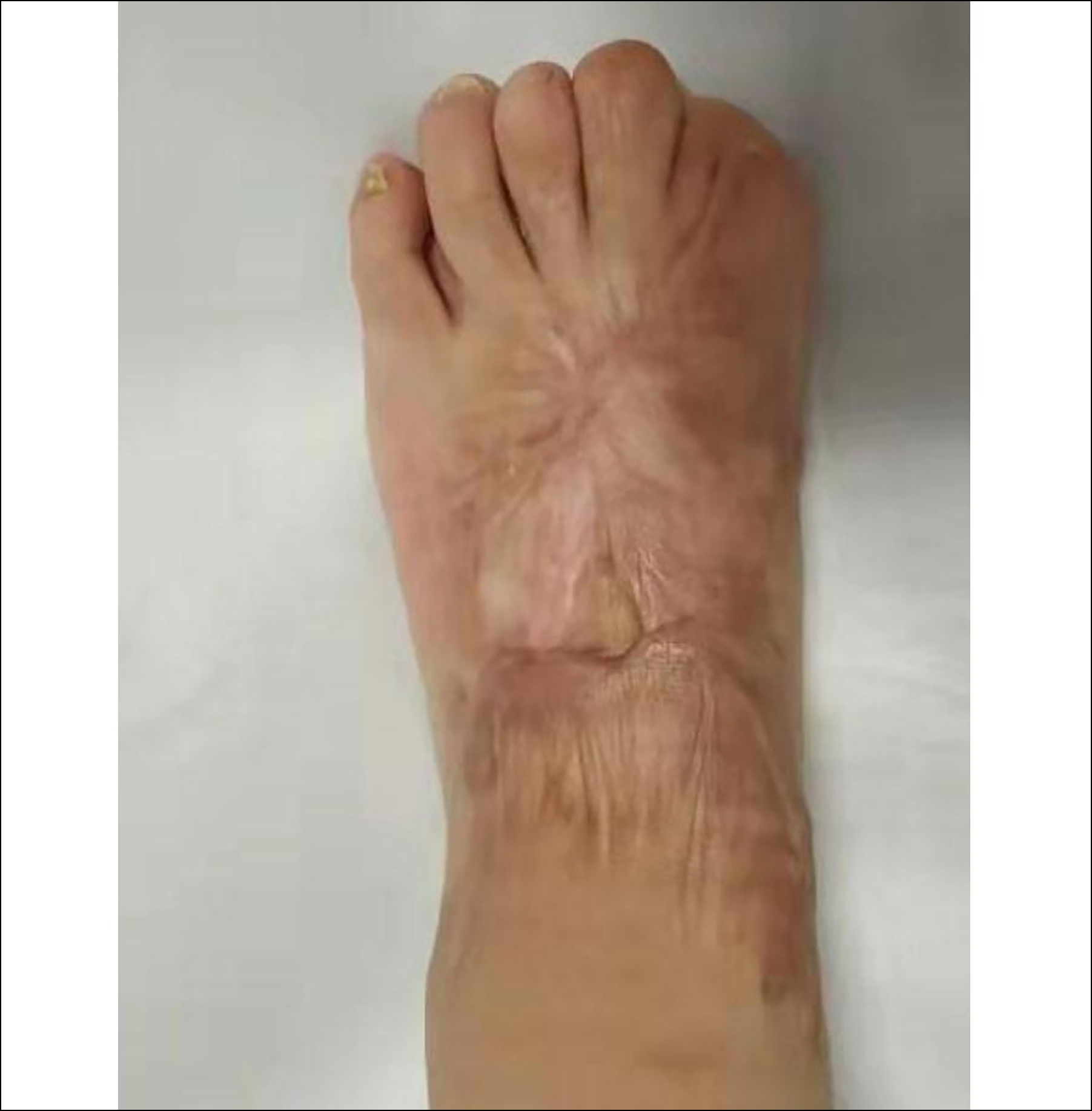 Figure 2: Follow-up at 110 days after the injury. The wound of the dorsum and toes 1-3 were healed, with partial scaring.
Figure 2: Follow-up at 110 days after the injury. The wound of the dorsum and toes 1-3 were healed, with partial scaring.
In this case, the child had a severe destructive injury to the left foot and ankle due to a traffic accident. After the surgery in ED, the entire foot developed extensive swelling, and the sole experienced massive ischemic necrosis. After a thorough evaluation of the child’s condition, we chose in-situ skin regeneration treatment. MEBO wound and ulcer dressing treatment effectively controlled infection of the wound. The inflammatory degeneration of the wound liquefied on its own, and non-invasive debridement was realized, while the granulation tissue of the wound remained moist.3,4 The regenerative potential of the cells and the physiological repair of the skin tissue were activated, which allowed the wound tissue to repair and heal itself without the need for skin grafting.
The results showed that the in-situ skin regeneration treatment was significantly superior to traditional Western medical therapy. The child had less pain, good compliance, a short wound healing time, and a good healing effect; therefore, this treatment method is worthy of clinical promotion.
ETHICAL APPROVAL:
Ethical approval was obtained from concerned quarters.
PATIENT’S CONSENT:
Written informed consent was obtained from the patient.
COMPETING INTEREST:
The authors declared no competing interest.
AUTHORS’ CONTRIBUTION:
GLHP: Manuscript preparation, literature review, contributed to the diagnosis, and provided clinical assistance.
XL, XC: Study design, manuscript correction, contributed to the diagnosis, and provided clinical assistance.
All authors approved the final version of the manuscript to be published.
REFERENCES
- Dang DY, McGarry SM, Melbihess EJ, Haytmanek CT, Stith AT, Griffin MJ, et al.Comparison of single-agent versus 3-additive regional anesthesia for foot and ankle surgery Foot Ankle Int 2019; 40(10): 1195-202. doi: 10.1177/10711007 19859020.
- MacNeill AL, Mayich DJ. Wide-awake foot and ankle surgery: A retrospective analysis Foot Ankle Surg 2017; 23(4): 307-10. doi: 10.1016/j.fas.2016.09.004.
- Lang YZ, Zhu HW, Zhang LN, Li JJ, Li H. Experience of applying MEBO wound & ulcer dressing in the treatment of diabetic ulcers. Chinese J Burns Wounds Surface Ulcers 2016; 28(11):34-7.
- EL-Hadidy MR, EL-Hadidy AR, Bhaa A, Asker SA, Mazroa SA. Role of epidermal stem cells in repair of partial-thickness burn injury after using moist exposed burn ointment (MEBO) histological and immune his to chemical study. Tissue Cell 2014; 46(2):144-51. doi: 10.1016/j.tice.2014. 01.002.