Superselective Renal Artery Embolization for Serious Renal Hemorrhage after Percutaneous Renal Biopsy in a Young Male
By Xiaodong Li1, Bingmu Liu2, Yancong Guo1Affiliations
doi: 10.29271/jcpsp.2023.03.365Sir,
Here, we report an unusual case of a young male with chronic nephritic syndrome who underwent percutaneous renal biopsy (PRB) guided by ultrasound and developed serious renal haemorrhage for several days, which was not controlled by conservative medical treatment. Thus, superselective renal artery embolisation (SRAE) was performed to treat the complication and the patient's renal bleeding stopped completely. SRAE is a secure and valid method for severe haemorrhage of kidney after PRB.
PRB is extensively performed for diagnosing and treating many kinds of kidney diseases in both native and transplanted kidneys.1 However, the procedure is not entirely risk-free. Bleeding is normally the most common complication due to the difficulty in compressing the biopsy site. Although the procedure’s adequacy and safety parameters have been obviously improved by ultrasound guidance and automatical puncturing biopsy systems,2 the incidence rate of gross hematuria is about 5% – 12% and the majority of patients with kidney haemorrhage are controlled with conservative treatment, such as resting, hemostatic medication and even blood transfusion.3 The rate of serious complications resulting in patient death has declined from 0.12 to 0.02%. Post-biopsy serious renal haemorrhage is unusual but a serious or even deadly complication.4 Currently, therapy for post-biopsy renal bleeding mainly involves hemostatic drugs, surgical repair and kidney resection. However, SRAE might be the preferred method in selected cases.5
A 16-year male patient with chronic nephritic syndrome was admitted to our hospital for PRB. On the next day, PRB was performed on the right side. The whole procedure was performed under ultrasound guidance, and the biopsy material was obtained successfully. However, continuous gross hematuria followed for the next several days after the procedure. It was not significantly improved by conservative medical treatment and was associated with a decline in haemoglobin levels. SRAE was conducted by a digital subtraction angiographic unit via the right femoral access by a 5 French (Fr.) catheter, five days later. A micro catheter (5 Fr, Terumo Medical, Japan) was used for superselective catheterisation in the right renal artery. Finally, arteriovenous fistula near the right inferior renal branch artery was diagnosed (Figure 1). As the injury site was discovered, the bleeding artery to the injury site was placed with a catheter (3 Fr, Terumo Medical, Japan) and four platinum coils (Tornado Embolisation Coils, Cook, CA, USA) were used for embolizing the lesions. Renal angiography was conducted for confirming the complete occlusion in the damaged vascular area and ended the entire operation (Figure 2). No complications occurred in the whole process. The patient's renal bleeding disappeared entirely and his haemoglobin values were distinctly improved 3 days after the procedure. Furthermore, no obvious changes in his renal functions after embolization were seen compared with preoperative renal functions.
This case demonstrates that SRAE can be a safe and valid choice for post-biopsy bleeding. Moreover, this endovascular technique may provide optimal protection of renal function too. If conservative treatment is ineffective for post-biopsy serious renal haemorrhage, SRAE should be considered and performed as early as possible.
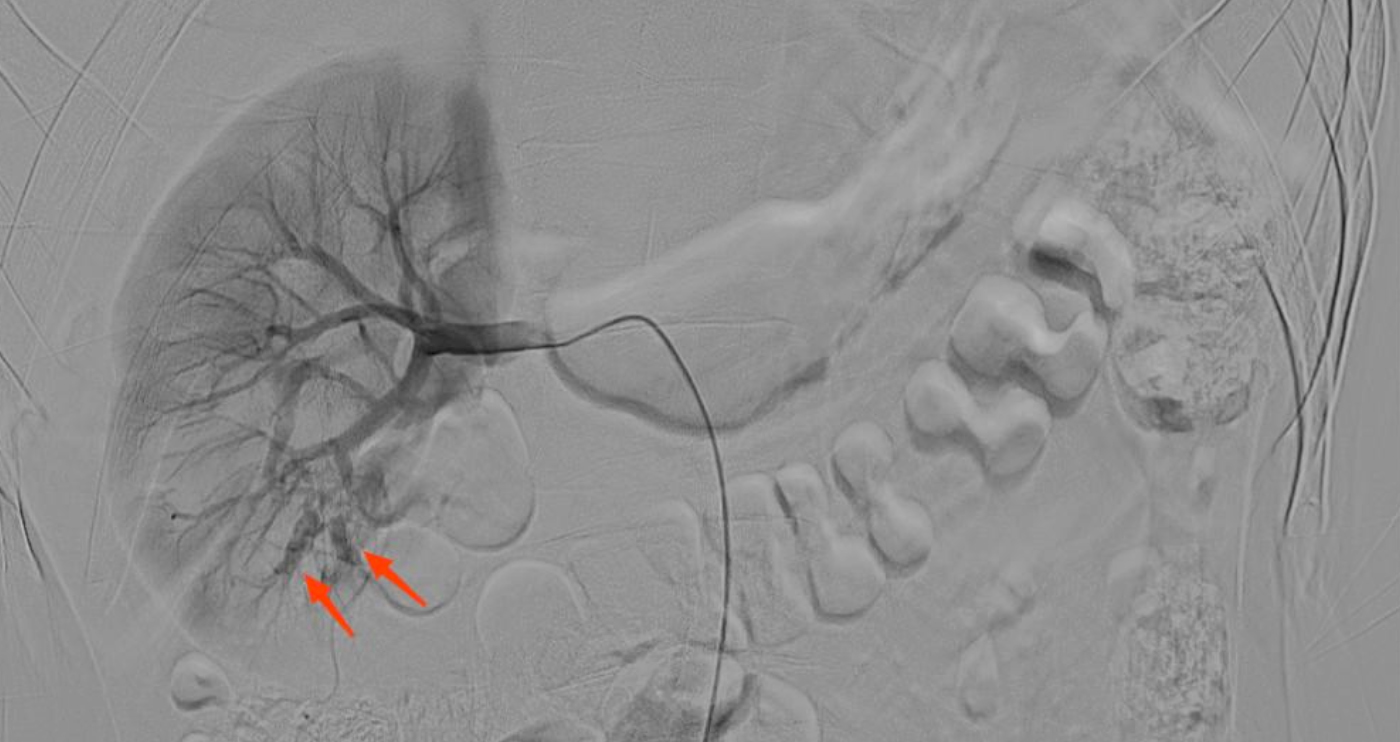 Figure 1: Right renal angiography showing contrast medium spilling out of the inferior lobar arteries.
Figure 1: Right renal angiography showing contrast medium spilling out of the inferior lobar arteries.
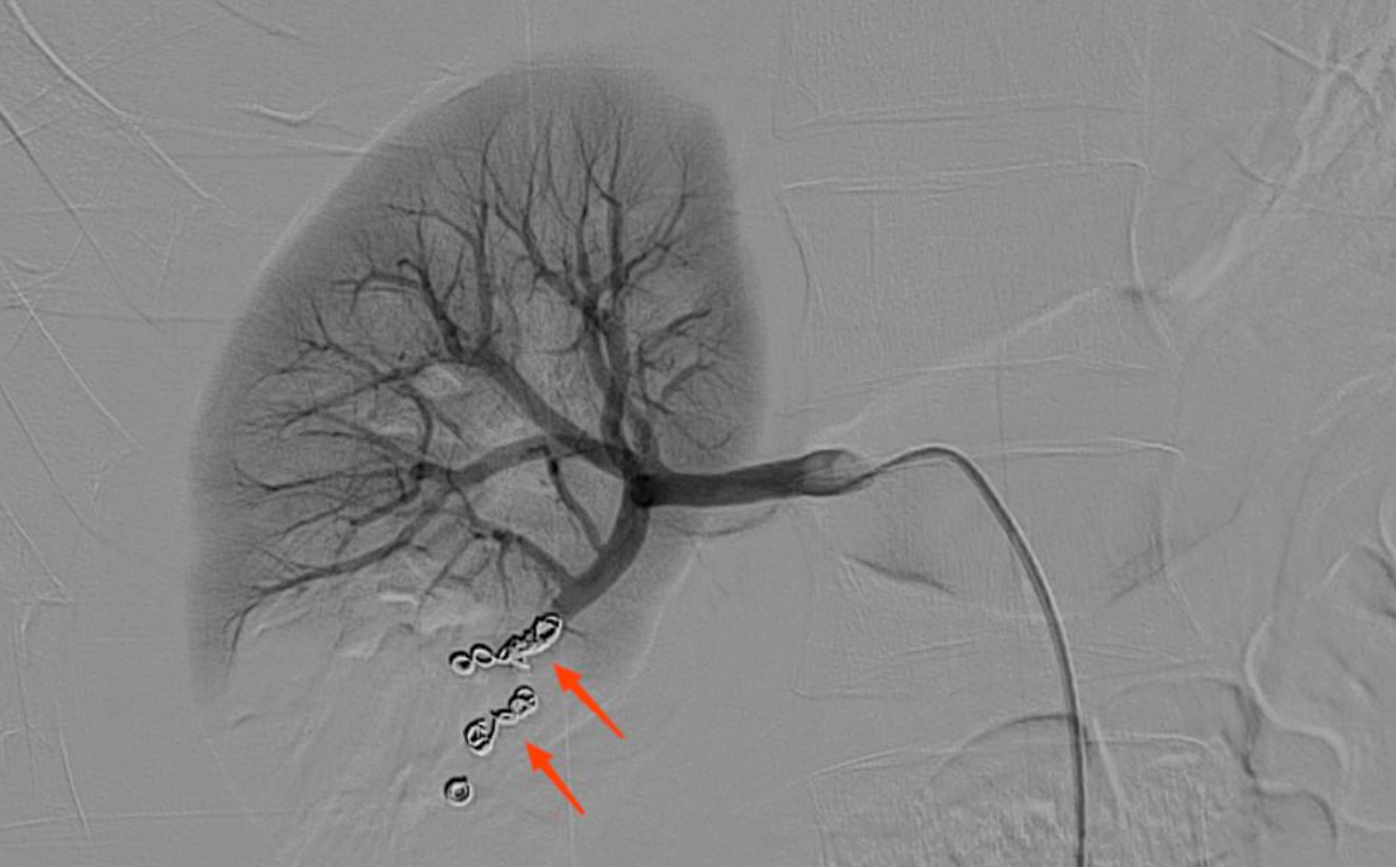 Figure 2: Post-embolisation angiography showed that the hemorrhage was disappeared and the injured artery and related site of kidney were occluded completely.
Figure 2: Post-embolisation angiography showed that the hemorrhage was disappeared and the injured artery and related site of kidney were occluded completely.
COMPETING INTEREST:
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential competing interest.
AUTHORS’ CONTRIBUTION:
XL: Manuscript writing, study design, and manuscript revision.
BL: Formulating patient’s treatment.
YG: Data collection.
All the authors contributed to the article and approved the submitted version.
REFERENCES
- Gutman T, Lopez-Vargas P, Manera KE, Craig JC, Howell M, Tunnicliffe D, et al. Identifying and integrating patient and caregiver perspectives in clinical practice guidelines for percutaneous renal biopsy. Nephrology (Carlton) 2019; 24(4):395-404. doi: 10.1111/nep.13406.
- Bakdash K, Schramm KM, Annam A, Brown M, Kondo K, Lindquist JD. Complications of percutaneous renal biopsy. Semin Intervent Radiol 2019; 36(2):97-103. doi: 10. 1055/s-0039-1688422.
- Zeng D, Liu G, Sun X, Zhuang W, Zhang Y, Guo W, et al. Transarterial embolisation for serious renal hemorrhage following renal biopsy. J Xray Sci Technol 2013; 21(3): 401-7. doi: 10.3233/XST-130391.
- Monahan H, Gunderson T, Greene E, Schmit G, Atwell T, Schmitz J. Risk factors associated with significant bleeding events after ultrasound-guided percutaneous native renal biopsies: A review of 2204 cases. Abdom Radiol (NY) 2019; 44(6):2316-22. doi: 10.1007/s00261-019-01962-z.
- Haochen W, Jian W, Li S, Tianshi L, Xiaoqiang T, Yinghua Z. Superselective renal artery embolisation for bleeding complications after percutaneous renal biopsy: A single-center experience. J Int Med Res 2019; 47(4):1649-59. doi: 10.1177/0300060519828528.