Mini Anterior Incision versus Conventional Incision in Thyroid Operations
By Mustafa Omer Yazıcioglu, Servet Kocaoz, Birol KorukluogluAffiliations
doi: 10.29271/jcpsp.2022.06.789ABSTRACT
Objective: To analyse the results of mini anterior incision compared to conventional Kocher’s incision in total thyroidectomy.
Study Design: Observational cohort study.
Place and Duration of Study: Department of General Surgery, Breast, and Endocrine Surgery Clinic, Ankara City Hospital, Turkey, from March 2019 to December 2019.
Methodology: Four hundred and twenty-five patients who underwent total thyroidectomy (TT) were divided into two groups; 132 patients in group 1 (mini anterior incision group) and 293 patients in group 2 (conventional incision group). Patient examination and follow-up findings were obtained from the hospital information system software (HIS). A questionnaire to verify the satisfaction of patients on different parameters was also completed by the researcher.
Results: Mini anterior incision significantly reduced incision length, scar thickness, discharge time, time to get back to work (p <0.001, p <0.001, p = 0.027, and p = 0.006, respectively). There was also less pain in the neck or surgical area in group 1 and less explicit or inconspicuous scar (p = 0.001 and p <0.001, respectively). Patients in group 1 found their surgery more aesthetic (p = 0.001). Central lymph node dissection (CLND) was performed in 21.31% of the patients with thyroid cancer in group 1.
Conclusion: More aesthetic results can be obtained by performing wound lip excision using a mini anterior incision. By using a mini anterior incision, CLND can be performed as effectively as with conventional incision in thyroid operations.
Key Words: Minimally invasive thyroid surgery, Mini anterior incision, Thyroidectomy, Cosmetic surgery.
INTRODUCTION
The morbidity and mortality of thyroid surgery operations have decreased due to the developing surgical techniques and devices. In thyroid surgery, surgeons focus on strategies that minimise pain, shorten hospital stay, and improve cosmetic results. For this reason, minimally invasive thyroidectomy (MIT) techniques have been developed.1-3 In addition to open operations, video-assisted endoscopic thyroidectomy (MIVAT) techniques achieved with cervical or extra-cervical incision have been applied.3-6 In open techniques, thyroidectomy is performed with an anterior or lateral incision, shortening the classical incision of Theodore Kocher by 2-3 cm. In these operations, better cosmetic results are obtained compared to classical open surgery. Therefore, an increase in thyroid surgery operations has been observed with the use of MIT techniques.7,8
The length of skin incision in the MIT technique ranges from 1.5 to 5 cm, depending on the surgeon's experience, the size of thyroid tissue, and nodule size. Extra cervical endoscopic approaches have the advantage of avoiding a cervical incision. MIVAT has the same results as anterior mini-incision.
However, the MIVAT technique requires a more comprehensive dissection than conventional surgery, the operation takes longer, and additional instruments are needed that increase cost.9,10 The aim of this study was to share the mini anterior incision experiences and investigate the cosmetic and other results, leading to better cosmetic and patient outcomes.
METHODOLOGY
It was a cross-sectional study conducted between March and December 2019 at the Department of General Surgery, Breast, and Endocrine Surgery Clinic, Ankara City Hospital. This cohort study is a mixed type which includes retrospective evaluation and prospective control of patients who were subjected to TT in the Hospital. Patients who underwent unilateral thyroid lobectomy, complementary thyroidectomy, lateral neck dissection, and parathyroidectomy were excluded. Amongst these dates, 543 patients underwent total thyroidectomy with or without CLND and lateral neck dissection (LND). Nine patients were excluded from the study due to lack of data.
The other 98 patients did not want to participate in the study. Eleven patients with lateral neck dissection were also excluded. The remaining 425 patients included in the study were called for, and a control examination was performed. Informed consent was taken from all patients before the control examination. Afterward, the researcher physician filled in the patient follow-up and evaluation form. Surgery reports, histopathology reports, and pre-and postoperative assessments of the patients were obtained from the hospital information system software with Hospital's permission.
Routine preoperative preparations were done in the outpatient clinic for the patients enrolled to undergo surgery. In addition, vocal cords were evaluated by indirect laryngoscopy of all patients before thyroid surgery and those patients who still had hoarseness or tone impairment three months after surgery.
The patients were divided into two groups, 132 patients were in group 1 (mini anterior incision group), and 293 patients were in group 2 (conventional incision group). The main differences of mini anterior incision from conventional incision were that a 2-4 cm incision was made 2-2.5 cm above the sternal notch depending on the size of the thyroid nodule. A traction suture was not placed on the upper flap to avoid narrowing the working area. Depending on the level of the skin incision, the upper pole or the lower pole, whichever was easier to reach, was started first. The wound lips, which were irritated by retraction, the thermal effect of cautery devices, and vessel sealing devices, were refreshed with a 2-3 mm cheek excision. The other steps of the operation were the same as conventional operation. Intraoperative neuromonitoring was routinely used in operations.
Scar evaluation was performed at least six months after surgery. The researcher physician who conducted the study asked the patients whether they were pleased about their incision, whether they found their surgery aesthetic, and whether they felt pain in their surgical area or neck.
The data was analysed in the SPSS (25.0, IBM Corp., Armonk, NY) program. Number, percentage, arithmetic mean, and standard deviation were used as descriptive statistics. The Kolmogorov-Smirnov test was checked to see if the data were normally distributed. The difference between the groups in terms of age was analysed with Student’s t-test. The age of the patients showed a normal distribution. It was found that thyroidectomy incision length, scar tissue thickness, postoperative discharge time, and go back to work time data were not normally distributed. The relationship between non-parametric continuous variables was analysed by using the Mann-Whitney U-test. Continuity Correction and Pearson Chi-square tests were used to compare the categorical variables of the patients. The statistical significance level was accepted as p <0.05.
RESULTS
The comparison of non-categorical parameters between two operation techniques is given in Table I. There is no significant difference between age, gender, type of surgery, hematoma, seroma development, infection development, and hypoparathyroidism in both groups (Table II).
One patient with conventional thyroidectomy had a tracheostomy due to bilateral vocal cord paralysis. The vocal cords were bilaterally mobile in the indirect laryngoscopic examination three weeks after treatment for this patient. The unilateral vocal cord was found to be fixed in paramedian in 1 (0.76%) of the patients in groups 1 and 4 (1.37%) of the patients in group 2 three months after the surgery.
The operation incision was extended to provide bleeding control in 2 (1.49%) of the patients in group 1, and the operation was transformed into conventional thyroidectomy. CLND was performed in 13 (21.31%) patients in group 1 and 26/115 (22.61%) patients in group 2.
Tumour diameter was more than 2 cm in 7 (53.85%) of these patients, and tumour diameter was measured as ≥3.5 cm in 4 (30.77%) patients in group 1. Lymph node metastasis was detected in 5/13 (38.46%) of patients in group 1 and 8/26 (30.77%) of patients in group 2 in histopathological examination. In group 1 , 13.64 ± 1.57 lymph nodes were detected in the histopathological examination of the cases, whereas 14.00 ± 2.45 lymph nodes were detected in t group 2 (p = 0.959).
When asked the patients whether the operation was aesthetic or not, it was found significantly more aesthetic in group 1 (p = 0.001, Figure 1). Likewise, in the physical examination performed at a distance of 5 meters, there were significantly less prominent or unnoticed scars in group 1 (p <0.001).
DISCUSSION
MIT surgery can be performed easily in nodular goitre cases with a thyroid nodule diameter less than 4 cm, in patients with Hashimoto's thyroiditis and Graves' disease with a thyroid volume of less than 30 cc. It is also recommended in follicular neoplasia cases smaller than 4 cm and in
patients with well-differentiated thyroid cancer less than 2 cm cancer size.11 In this study, in 13 cases, the longitudinal length of the nodule was more than 4 cm. Due to the cystic structure of the thyroid nodules, the operation was successfully performed by pulling the thyroid lobe out through the small incision. Likewise, in more than half of the cases with well-differentiated thyroid cancer, MIT surgery was also successfully performed, although the tumour diameter was more than 2 cm.
Indications for the use of MIT surgery have been expanded, including differentiated thyroid cancers with lymph node involvement, in specialized surgery centres.12 This study showed that CLND could be accomplished through an MIT incision. In addition, there was no significant difference between the number of lymph nodes removed in CLND between group 1 and group 2.
It may be necessary to convert the surgery to conventional thyroidectomy in 5% of patients in MIT surgery.13 In this study, this rate was found to be 1.49%. The mini anterior incision is also easy to convert to the conventional incision when it is required. Furthermore, the mini anterior technique can be performed with the same instruments as in conventional thyroidectomy, which does not increase surgery costs.
Table I: Comparison of some categorical and continuous parameters with the operation technique.
|
|
Group 1 |
Group 2 |
p-value |
||
|
Mean |
SD |
Mean |
SD |
||
|
Patient age |
49.41 |
12.75 |
49.03 |
12.36 |
0.822* |
|
|
Median |
IQR |
Median |
IQR |
|
|
Discharge time (days) |
2.5 |
1 |
3 |
1 |
0.027 |
|
Back to work time (days) |
1 |
2 |
3 |
11 |
0.006 |
|
Incision length (cm) |
4 |
1 |
6 |
5 |
0.000 |
|
Scar tissue width. |
1 |
1 |
1 |
1 |
0.000 |
|
Preoperative USG Nodule diameter |
15 |
15 |
20 |
27.2 |
0.068 |
|
SD: Standard deviation, IQR: Interquartile range, Student’s t-test *, Mann-Whitney U-test are used. |
|||||
Table II: Comparison of surgical technique with categorical parameters.
|
|
Surgical technique |
p-value |
|||
|
Group 1 |
Group 2 |
||||
|
Gender |
Male |
n |
32 |
62 |
0.479 |
|
% |
34.0 |
66.0 |
|||
|
Female |
n |
100 |
231 |
||
|
% |
30.2 |
69.8 |
|||
|
Operation type |
TT |
n |
119 |
267 |
0.747 |
|
% |
30.8 |
69.2 |
|||
|
TT+CLND |
n |
13 |
26 |
||
|
% |
33.3 |
66.7 |
|||
|
Presence of infection |
No |
n |
126 |
283 |
0.770 |
|
% |
30.8 |
69.2 |
|||
|
Yes |
n |
6 |
10 |
||
|
% |
37.5 |
62.5 |
|||
|
Presence of hematoma and/or seroma |
No |
n |
123 |
267 |
0.601 |
|
% |
31.5 |
68.5 |
|||
|
Yes |
n |
9 |
26 |
||
|
% |
25.7 |
74.3 |
|||
|
Hypoparathyroidism |
Not seen |
n |
103 |
217 |
0.670 |
|
% |
32.2 |
62.8 |
|||
|
Temporary hypoparathyroidism |
n |
24 |
64 |
||
|
% |
27.3 |
72.7 |
|||
|
Permanent hypoparathyroidism |
n |
5 |
12 |
||
|
% |
29.4 |
70.6 |
|||
|
Hoarseness |
No |
n |
105 |
204 |
0.034 |
|
% |
34.0 |
66.0 |
|||
|
Yes |
n |
27 |
89 |
||
|
% |
23.3% |
76.7% |
|||
|
Pain in the surgical area |
No |
n |
126 |
247 |
0.002* |
|
% |
33.8 |
66.2 |
|||
|
Yes |
n |
6 |
46 |
||
|
% |
11.5 |
88.5 |
|||
|
Is your surgery aesthetic? |
Not aesthetic |
n |
5 |
51 |
0.001* |
|
% |
8.9 |
91.1 |
|||
|
Undecided |
n |
31 |
64 |
||
|
% |
32.6 |
67.4 |
|||
|
Aesthetic |
n |
96 |
178 |
||
|
% |
35.0 |
65.0 |
|||
|
Scar inspection for 5 meters |
No obvious scar |
n |
89 |
126 |
<0.000 |
|
% |
41.4 |
58.6 |
|||
|
Incision scar is visible |
n |
43 |
167 |
||
|
% |
20.5 |
79.5 |
|||
|
Total |
|
n |
132 |
293 |
0.002* |
|
% |
31.1 |
68.9 |
|||
|
n: Number, Pearson Chi-square test, and continuity correction test * were used. |
|||||
In the previous MIT series, the postoperative hospitalization period was reported shorter than conventional thyroidectomy.14 In this study, the duration of hospital stay and back to work time was shorter for patients in the mini anterior technique. Postoperative pain and skin complications are less common in mini anterior incisions as with less dissection without creating a large skin flap.14,15 Postoperative pain was significantly lower in patients with the mini anterior technique. In addition, it was shown smaller and less explicit scar in the MIT technique with a mini anterior incision.11,16 The scar was less noticeable and more difficult to see when viewed from a distance.
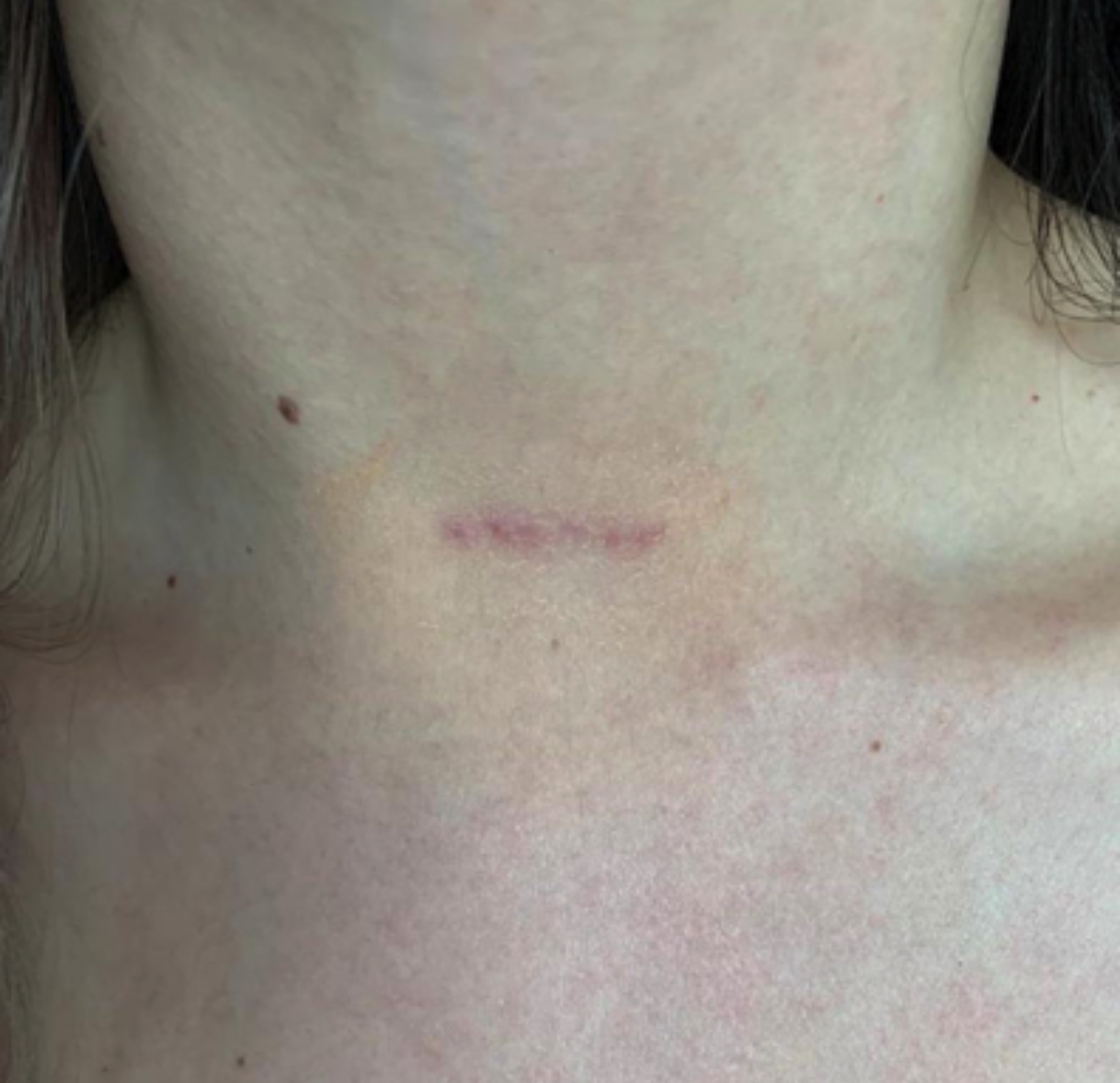 Figure 1: Operated patient with mini anterior incision, the postoperative 6th month
Figure 1: Operated patient with mini anterior incision, the postoperative 6th month
Previous studies have reported that the temporary RLNP rate was 3.92-10.6% and permanent RLNP in 0.89-1.1%.17-19 Dionigi et al. have reported that 96.2% of cases with postoperative RLNP fully recovered within 6-12 months.19 In this study, temporary RLNP was observed in 20.45% and permanent RLNP in 0.75% of patients with mini anterior incisions.
Although conventional thyroidectomy is the gold standard in thyroid surgery, the mini anterior technique increases patient satisfaction due to small incisions, less dissection area, better cosmetic results, and less postoperative pain. It also makes it easier for patients to make thyroid surgery decisions.11-16 Linos et al. have reported that patients undergoing mini incisions were cosmetically pleased, and 81.2% would not prefer trans-axillary MIVAT surgery.8 Of the patients, 93.44% were satisfied with the operation in the mini-incision group.
One of the possible weaknesses of this study may be that scar assessment was not evaluated with a standard scale. This was due to standard rating scales for postsurgical scar assessments takes time, and most patients' control examinations coincided with the novel COVID-19 pandemic. Although the present study showed that central lymph node dissection could be performed with a mini anterior incision, the lack of long-term oncological results may be one of the weaknesses of this study.
CONCLUSION
The mini anterior incision is smaller and less explicit. Length of hospital stay and back to work time was shorter than the conventional incision. Patients experienced less pain in the neck or surgical area in the mini anterior incision technique. Better aesthetic results can be obtained by wound lip excision in mini anterior incision surgery. TT and CLND can also be performed effectively as conventional surgery in patients with the mini anterior incision technique. In conclusion, mini anterior incision is a preferred MIT technique due to its low complication rate and aesthetic results.
ETHICAL APPROVAL:
The study was approved by Ankara City Hospital 1. Clinical Research Ethics Committee (Decision No. E-19-111, date: 24.12.2019).
PATIENTS’ CONSENT:
Informed consent was taken from all patients who participated in this study.
COMPETING INTEREST:
The authors declared no competing interest.
AUTHORS’ CONTRIBUTION:
MOY: Concept, design, literature review, data collection, writer.
SK: Concept, design, data collection, data analysis, literature review.
BK: Supervisor, concept, data analysis, critical review.
All authors approved the final version of the manuscript to be published.
REFERENCES
- Ruggieri M, Straniero A, Maiuolo A, Pacini FM, Chatelou E, Batori M, et al. The minimally invasive surgical approach in thyroid diseases. Minerva Chir 2007; 62(5):309-14.
- Stalberg P, Delbridge L, Van Heerden J, Barraclough B. Minimally invasive parathyroidectomy and thyroidectomy - current concepts. Surgeon 2007; 5(5):301-8. doi: 10.1016/ s1479-666x(07)80029-1.
- Vidal O, Saavedra-Perez D, Vilaça J, Pantoja JP, Delgado-Oliver E, Lopez-Boado MA, et al. Minimally-invasive endocrine neck surgery. Cir Esp 2019; 97(6):305-13. doi: 10.1016/j.ciresp.2019.03.010.
- Palazzo FF, Sebag F, Henry JF. Endocrine surgical technique: Endoscopic thyroidectomy via the lateral approach. Surg Endosc 2006; 20(2):339-42. doi: 10.1007/s00464- 005- 0385-1.
- Miccoli P, Ambrosini CE, Materazzi G, Fregoli L, Fosso LA, Berti P. New technologies in thyroid surgery. Endoscopic thyroid surgery. Minerva Chir 2007; 62(5):335-49.
- Ruggieri M, Straniero A, Mascaro A, Genderini M, D'Armiento M, Gargiulo P, et al. The minimally invasive open video-assisted approach in surgical thyroid diseases. BMC Surg 2005; 5:9. doi: 10.1186/1471-2482-5-9.
- Cavicchi O, Piccin O, Ceroni AR, Caliceti U. Minimally invasive nonendoscopic thyroidectomy. Otolaryngol Head Neck Surg 2006; 135(5):744-7. doi: 10.1016/j.otohns. 2006.06. 1246.
- Linos D, Economopoulos KP, Kiriakopoulos A, Linos E, Petralias A. Scar perceptions after thyroid and parathyroid surgery: Comparison of minimal and conventional approaches. Surgery 2013; 153(3):400-7. doi: 10.1016/j. surg.2012.08.008.
- Runge T, Inglin R, Riss P, Selberherr A, Kaderli RM, Candinas D, et al. The advantages of extended subplatysmal dissection in thyroid surgery-the "mobile window" technique. Langenbecks Arch Surg 2017; 402(2):257-63. doi: 10.1007/ s00423-016-1545-6.
- Byeon HK, Holsinger FC, Tufano RP, Chung HJ, Kim WS, Koh YW, et al. Robotic total thyroidectomy with modified radical neck dissection via unilateral retroauricular approach. Ann Surg Oncol 2014; 21(12):3872-5. doi: 10.1245/s10434-014- 3896-y.
- Sabuncuoglu MZ, Sabuncuoglu A, Sozen I, Benzin MF, Cakir T, Cetin R. Minimally invasive surgery using mini anterior incision for thyroid diseases: A prospective cohort study. Int J Clin Exp Med 2014; 7(10):3404- 09.
- Dralle H, Machens A, Thanh PN. Minimally invasive compared with conventional thyroidectomy for nodular goitre. Best Practice Res Clin Endocrinol Metabolism 2014; 28(4):589-99. doi: 10.1016/j.beem.2013.12.002.
- Dobrinja C, Trevisan G, Makovac P, Liguori G. Minimally invasive video-assisted thyroidectomy compared with conventional thyroidectomy in a general surgery department. Surg Endosc 2009; 23(10):2263-7. doi: 10.1007/s00464-008- 0303-4.
- Henry JF. Minimally invasive thyroid and parathyroid surgery is not a question of length of the incision. Langenbecks Arch Surg 2008; 393(5):621-6. doi: 10.1007/s00423-008-0406-3.
- Park CS, Chung WY, Chang HS. Minimally invasive open thyroidectomy. Surg Today 2001; 31:665-9. doi: 10.1007/ s005950170066.
- Terris DJ, Seybt MW, Elchoufi M, Chin E. Cosmetic thyroid surgery: Defining the essential principles. Laryngoscope 2007; 117(7):1168-72. doi: 10.1097/MLG.0b013e318053 db8f.
- Tartaglia F, Russo G, Sgueglia M, Blasi S, Tortorelli G, Tromba L, et al. Total thyroidectomy in geriatric patients: A retrospective study. Int J Surg 2014; 12 Suppl 2:S33-S36. doi: 10.1016/j.ijsu.2014.08.386.
- Joliat GR, Guarnero V, Demartines N, Schweizer V, Matter M. Recurrent laryngeal nerve injury after thyroid and parathyroid surgery: Incidence and postoperative evolution assessment. Medicine (Baltimore) 2017; 96(17):e6674. doi: 10. 1097/MD.0000000000006674.
- Dionigi G, Wu CW, Kim HY, Rausei S, Boni L, Chiang FY. Severity of recurrent laryngeal nerve injuries in thyroid surgery. World J Surg 2016; 40(6):1373-81. doi: 10.1007/ s00268-016-3415-3.