Could “Retrograde Intrarenal Surgery” be Used as an Efficient Technique in the Treatment of Calyceal Diverticula Stones
By Basri Cakiroglu1, Tuncay Tas2, Suleyman Hilmi Aksoy3, Ersan Arda4Affiliations
doi: 10.29271/jcpsp.2022.05.623ABSTRACT
Objective: To evaluate the efficacy of retrograde intrarenal surgery (RIRS) and holmium laser lithotripsy in the treatment of symptomatic renal calyceal diverticular (CD) stones.
Study Design: A case series.
Place and Duration of Study: Department of Urology, Hisar Intercontinental Hospital, from 2008 and 2019.
Methodology: Patients who underwent holmium laser lithotripsy with RIRS to manage symptomatic CD stones were evaluated retrospectively. Demographics, stone size, operation and hospital stay duration, the success of treatment and complications were noted.
Result: Among the 30 treated patients, 13 patients were female and 17 were male. The mean age was 45.4 ± 11.9 (26-64), the stone diameter was 14.4 ± 4.1 mm, operation time was 70.47±35.7 (35-155) minutes, and mean length of hospital stay was 1.27±0.5 (1-3) days. In those patients who underwent RIRS, 26 (86.7%) were successfully treated while in 4 of 30 patients (13.3%) the procedure was not successful. Complications were observed in 10 (33.3%) patients. Clavien-I complications were demonstrated in 6 patients, Clavien III complications were demonstrated in 3 patients. One patient had urosepsis, 2 patients had ureteral laceration, and one patient with Clavien IV complication had perirenal hematoma.
Conclusion: Laser lithotripsy therapy with RIRS is a safe and effective treatment for symptomatic calyceal diverticular stones and can be offered as the first-line treatment for calyceal diverticular stones.
Key Words: Calyceal diverticula, Stone disease, Flexible ureterorenoscopy, Holmium laser, RIRS.
INTRODUCTION
Calyceal diverticulum (CD) is a congenital or acquired abnormality that is characterized by a cystic space containing urine in the renal parenchyma surrounding the muscularis mucosa which is covered by transitional epithelium.1 CD is divided into two types: type 1 is the most common (and sometimes small in size) seen in the kidney poles, especially in the upper pole. Type 2 has a central location with direct communication to the collection system. Type II diverticulum is larger, tends to be symptomatic, and is more commonly located in the middle part of the kidney.1
CD is a rare disease and its incidence is unknown, but it has been reported in 0.21-0.6% of intravenous pyelographic examinations, and it has been demonstrated to be bilateral in approximately 3% of patients.2
In most of the cases, the pathology is unilateral (97%) and the most commonly involved part is the upper and middle pole of the kidney. CD is usually asymptomatic, but the patients may have pain, infection, stone formation, abscess formation, hematuria, and sepsis complications.3 It has been reported that the incidence of CD stone formation is 10—50%.4 Current minimally invasive treatments for patients with symptomatic CD stones include SWL, flexible ureterorenoscopy (RIRS), percutaneous nephrolithotomy (PCNL), and laparoscopy. It has been reported that PCNL and RIRS are the most successful treatment strategies in relevant patients.5-8 However, the success of these two treatments has not been fully demonstrated, and larger studies are needed. The success of these treatment methods required documentation.
The aim of this study was to evaluate the outcome of patients who underwent holmium laser with RIRS for symptomatic CD stones.
METHODOLOGY
This observational study was approved by the Hisar Intercontinental Hospital, University Medical Faculty Ethics Committee (Protocol No. 2020/434). All patient data were protected confidentially and in accordance with the Declaration of Helsinki.
Between 2008 and 2019, the data of 30 patients who underwent flexible ureteroscopic laser lithotripsy for CD stones and patients who developed stormy between diverticulum and calyx were retrospectively evaluated. The same experienced urologist performed all surgical procedures. Data regarding the patient's history, other demographic characteristics, comorbidities, and previous stone management history were assessed. Preoperative tomography and other radiological examinations were examined. Each patient underwent computed tomography scan (CT) before surgery to evaluate the stone and calyceal diverticulum. Normally, non-contrast computed tomography (NCCT) is performed for patients with renal stones, contrast tomography was only performed to those patients with suspected diverticula (Figure 1).
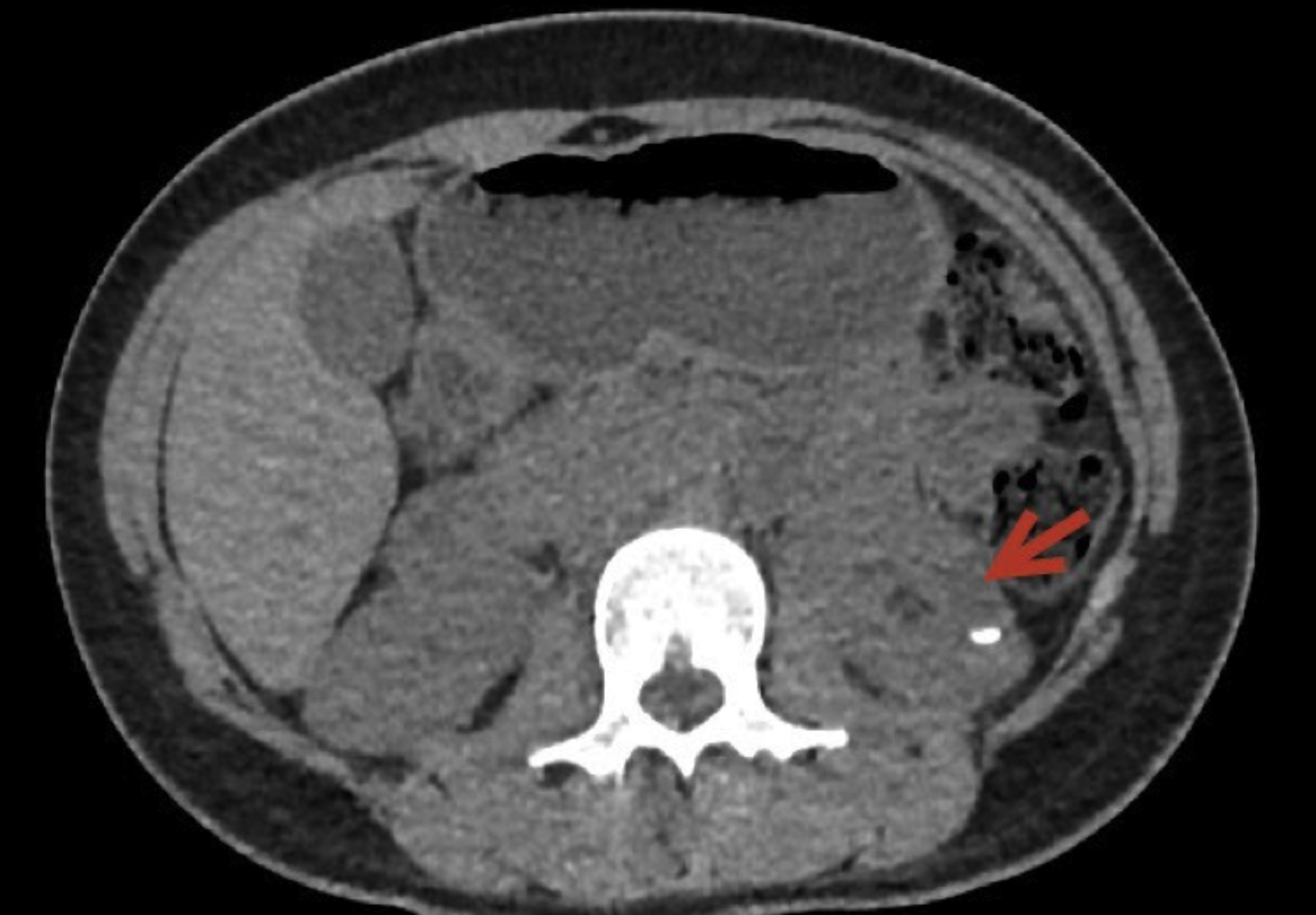 Figure 1: Plain CT image revealed a cystic lesion at the middle pole of the left kidney with stone inside.
Figure 1: Plain CT image revealed a cystic lesion at the middle pole of the left kidney with stone inside.
Routine blood biochemistry tests, urine analysis and urine culture tests were evaluated as preoperative diagnostic procedures. Operation time and surgical complications were evaluated perioperatively according to Clavien-Dindo calcification.
After the patients were placed in the lithotomy position under general anesthesia and the necessary regional cleaning was performed and covered, the urethra and bladder were examined under direct vision with 8 F ureteroscopy, after the ureteral orifice was seen, a 0.038 inch 145 cm safety guidewire was placed up to the relevant ureter and kidney. Then, 10 F access sheath was placed over the guidewire up to the upper ureter. All patients were treated with RIRS and holmium YAG laser lithotripsy. A flexible ureterorenoscope (Flex-X2, Karl Storz, Tuttlingen, Germany) and a 273 micron fiber holmium laser were used to break and / or remove stones from the CD. Holmium laser machine was adjusted to 1.0-1.5 J energy and 8-10 Hz speed. After laser lithotripsy, stone fragments larger than 3 mm were removed with a basket, fragments smaller than 3 mm were left for spontaneous dropping, especially after the diverticulum orifice was enlarged for the stones in the lower calyx, the stones were taken to the upper calyx and there they were fragmented with holmium laser.
A 4.8-F double J (DJ) ureteral catheter was then placed routinely in all patients and removed 4-6 weeks after the procedure. The top dressing of the stent was placed in the diverticulum to drain the urine and to prevent the diverticulum neck from collapsing and to ensure mucosal integrity.
Renal ultrasonography (US) or plain abdominal radiography of the kidney, ureter and bladder was performed at the 48th hour to evaluate the stone-free status and the location of the drainage tubes. Urinalysis, urine culture, kidney, ureter and bladder radiography and renal NCCT were performed 4 weeks after their discharge at the urology outpatient clinic. CD resolution NCCT was evaluated. Long-term follow-up of the patients was 3-6 months after the procedure, this assessment was based on the presence or absence of residual stone fragments, symptoms and complications. Depending on the presence of residual stone fragments (RF), symptoms, and complications long-term follow-up of patients was 3 to 6 months after the procedure.
SPSS 25.0 (Statistical Package for Social Sciences, Chicago, USA) program was used for all statistical evaluations. Descriptive statistics were presented as mean ± standard deviation (Mean ± SD) for continuous variables, and as numbers and percentages for categorical data.
Table I: Demographic characteristics and surgical statistics.
|
Variable |
Value |
|
Gender (n) Male Female Age (years) BMI (kg/m2) Stone burden (mm) Surgery time (min) Success rate Stone-free rate CIRF Hospitalization time (day) Complications Clavien I Clavien III Clavien IV |
17 13 45.4 ± 11.9 27.62 ± 2.73 14.4±4.09 70.47±35.7 86.7% 73.3% 13.3% 1.3±0.5
6(20%) 3(10% 1(3.3%) |
|
CIRF: Clinically insignificant residues. |
|
RESULTS
Thirty patients were included in the study, 13(43.3%) of them were female and 17(56.7%) of them were male. The mean age was 45.4 ± 11.9 (26-64) years. The mean body mass index was 27.61 ± 2.74 Kg/m2 with stones diameter of 14.4 ± 4.1 mm. The mean operation time was 70.47 ± 35.7 (35-155) minutes, and the mean duration of hospitalization was 1.27 ± 0.5 (1-3) days (Table I). Sixteen of the patients had previously undergone SWL, 2 percutaneous nephrolithotomy, and 2 URS operations due to kidney stones.
The diverticulum was located to the lower calyx in 6 (20%) patients, middle calyx in 10 (33.3%) patients, and upper calyx 14 (46.7%) patients. According to the stone analysis results, the most common stone composition was calcium oxalate stones 18(60%) of all stones) followed by calcium phosphate stones 7 (23.3%) of all stones), infectious stones 4(13.3%) of all stones), and one (3.3%) uric acid stone. A double J stent was placed in all patients.
After RIRS, 22 (73.3%) patients were stone-free (SF) and clinically insignificant residues (less than 4 mm) (CIRF) were demonstrated in 4 (13.3%) patients. Residual stone fragments were demonstrated in 4 (13.3%) patients. The success rate was accepted as SF or CIRF and achieved in 26 (86.7%) patients.
The complication was demonstrated in 10 (33.3%) patients. Twenty (66.7%) of the patients were complication-free. Clavien-I complication was demonstrated in 6 patients (4 stent pain, 2 gross hematuria), Clavien III complication was demonstrated in 3 patients (1 patient urosepsis, 2 ureteral lacerations), Clavien-IV complication was demonstrated in one patient (perirenal hematoma) (Table I). The patient with perirenal hematoma had a diverticulum in the lower pole and a 2.5 cm stone with a large diverticulum (Figure 2).
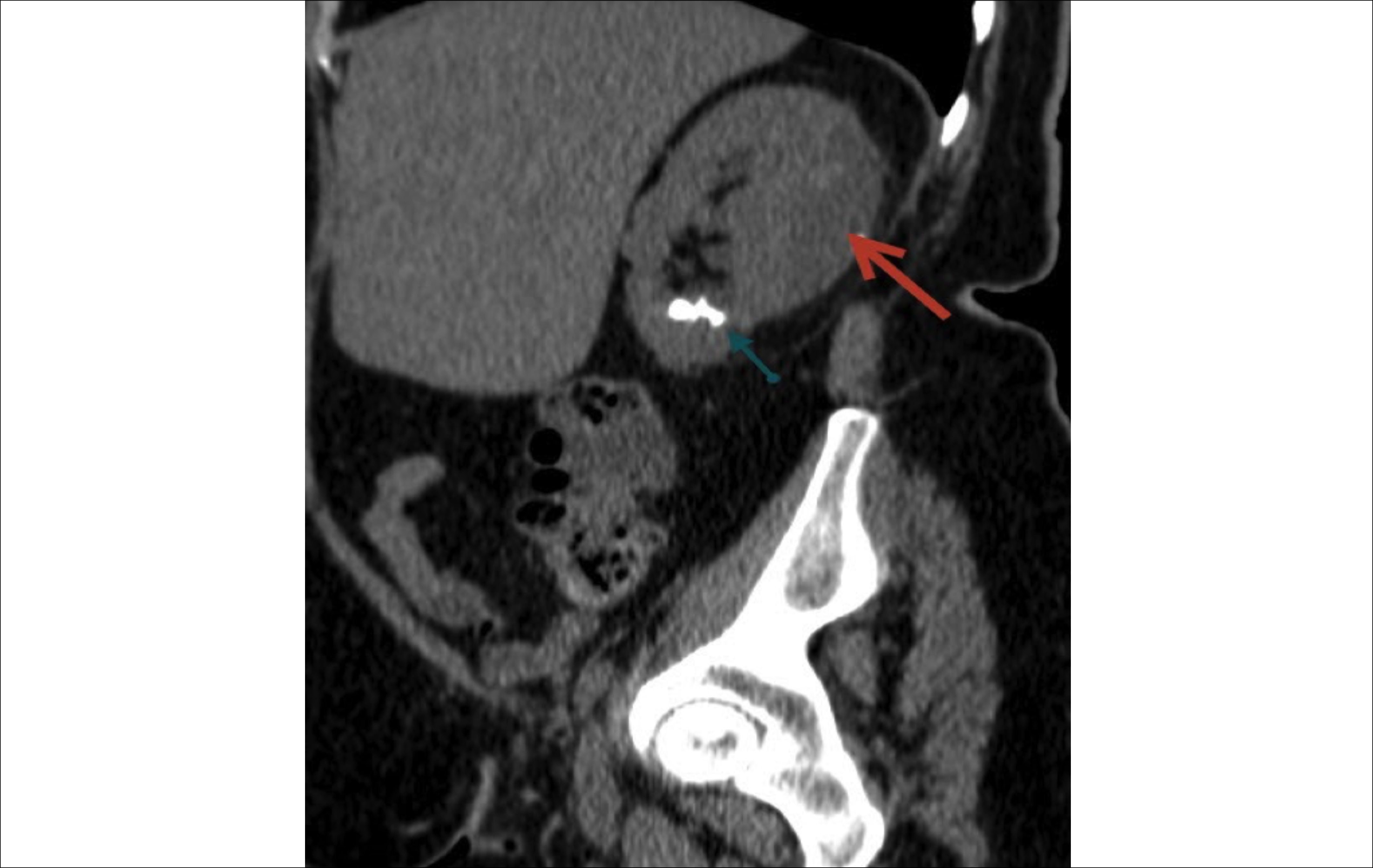 Figure 2: CT image of the perirenal hematoma after the RIRS operation and remaining residual stones.
Figure 2: CT image of the perirenal hematoma after the RIRS operation and remaining residual stones.
DISCUSSION
While RIRS has been used frequently for small stones in the upper or middle calyx CD, PCNL has been accepted as the first choice treatment strategy in patients with CD stones in recent years.9,10
RIRS is more effective than ESWL monotherapy in the treatment of DC stones. It is also less invasive than PCNL or laparoscopic approaches, regarding its feasibility most cases can be performed without hospitalization.5 PCNL is usually the preferred method because posterior CD stones are easy to access, but anterior CD stones can be difficult in terms of increased complications such as bleeding due to their longer distance.11,12
The results differ from the previous published studies in several aspects. The gender ratio of male patients was higher (56.7%) while in other studies the ratio of male patients was lower. Another difference is the location of diverticula. In general the location of the diverticula has been reported to be at the upper calyx with a rate of 37.5% to 70%, at the middle calyx 20% to 37.5%, and at the lower calyx 10% to 18.4%.4,13,14 In the most recent comprehensive evaluation, 48.9% of the diverticula were demonstrated to be at the upper calyx, 29.7% at the middle calyx, and 21.4% was at the lower calyx. These data correspond to the data of our series.12 In this patient group, 20% of the diverticula were located at the lower calyx, 33.3% at the middle calyx, and 46.7% at the upper calyx.
SF rates exceeding 85% were found in most studies for PCNL and SWL in the treatment of CD stones.2,15 In another review, the SF rate of 153 patients who underwent RIRS was reported as 61.4% and symptom-free rate as 67.9%.16 In this study, this rate was found to be 86.7% as a treatment success.
In a prospective study, Clavien I complication occurred in 11.4% of 35 patients treated with RIRS and no other complications were reported.17 In this study, Clavien-I complications were demonstrated in 6 patients, Clavien-III complications were demonstrated in three patients and one patient developed Clavien-IV complications. There were no Clavien-II complications reported. Clavien-IV complication was demonstrated in a patient with perirenal hematoma. Perirenal hematoma in RIRS is a condition that develops after fornix rupture, which occurs due to trauma in the pelvicalyceal system due to increased intrarenal pressure.18,19
Moderate-severe hydronephrosis, thin renal cortex, long operation time, hypertension, female gender and UTI could be counted among the risk factors of perirenal hematoma (PRH) in patients who underwent RIRS. Other risk factors include higher perfusion pressures, larger stone size, concurrent chronic kidney disease (CKD), pre- and postoperative ureteral stent use, ureteral sheath use, and previous kidney operation or SWL. The incidence of PRH development in RIRS is reported as 0.15% to 8.9%.20
The relevant patient had many of these risk factors, 49-year-old female patient, severe hydronephrotic lower pole diverticulum, 20 mm stone, 130 minutes of operation time, recurrent UTI and recurrent SWL.
Patients who develop PRH often have flank pain, fever, or a drop in haemoglobin. The hematoma was diagnosed with subsequent US or CT imaging. Most of the articles concluded that conservative therapy is the best initial treatment for PRH. The mortality rate of patients with PRH is reported to be 2.5%.19,20
Our patient also had flank pain, subfebrile fever and a decrease in haemoglobin in the postop period. US and CT were performed, it was found that there was a 45 × 25 mm diameter hematoma. There was no need for blood transfusion, daily hemogram and ultrasound follow-up was done. When the patient was haemodynamically stable, he was discharged on the 5th day, after about 3 months, the hematoma was completely resorbed.
Significant bleeding may occur during the incision of the diverticular neck that interferes with the surgeon's vision due to the proximity of the infundibular vessels. In that case the procedure should be terminated, and a stent should be placed. But in general, transfusion is rarely required. Arteriography and embolization should be considered if bleeding is persistent.21
Moderate bleeding occurred in 7 patients, which did not require the termination of the procedure. A double J stent was inserted in these patients. Renal arteriography and embolization were performed in only 1 patient after bleeding continued in the postoperative period and there was a significant decrease in haemoglobin.
CONCLUSION
RIRS and holmium laser are safe methods in the treatment approach of kidney stones. Their use is feasible and safe in the treatment of calyceal diverticular stones that are smaller lower than 2 cm in diameter. These treatment tools should be considered in clinical practice especially for their high rate of stone-free results and low rate of complications.
ETHICAL APPROVAL:
All procedures performed in the study involving human participants were in accordance with ethical standards. Trakya University Medical Faculty Ethics Committee approval was obtained prior to the study. Informed consent Informed consent was obtained from all individual participants included in the study.
COMPETING INTEREST:
The authors declared no conflict of interest.
AUTHORS’ CONTRIBUTION:
BC: Literature review, writer, conception, design, supervision and critical review.
TT: Literature review, analysis and interpretation.
SHA: Data collection, processing, conception and design.
EA: Supervision and critical review.
All authors approved the final version of the manuscript to be published.
REFERENCES
- Wulfsohn MA. Pyelocaliceal diverticula. J Urol 1980; 123(1): 1-8. doi: 10.1016/s0022-5347(17)55748-1.
- Gross AJ, Herrmann TR. Management of stones in calyceal diverticulum. Curr Opin Urol 2007; 17(2):136-40. doi: 10. 1097/MOU.0b013e328011bcd3.
- Ding X, Xu ST, Huang YH, Wei XD, Zhang JL, Wang LL, et al. Management of symptomatic caliceal diverticular calculi: Minimally invasive percutaneous nephrolithotomy versus flexible ureterorenoscopy. Chronic Dis Transl Med 2016; 2(4): 250-6. doi: 10.1016/j.cdtm.2016.11.016.
- Timmons JW Jr, Malek RS, Hattery RR, Deweerd JH. Caliceal diverticulum. J Urol 1975; 114(1):6-9. doi: 10.1016/ s0022-5347(17)66930-1.
- Sejiny M, Al-Qahtani S, Elhaous A, Molimard B, Traxer O. Efficacy of flexible ureterorenoscopy with holmium laser in the management of stone-bearing caliceal diverticula. J Endourol 2010; 24(6):961-7. doi: 10.1089/end.2009.0437.
- Smyth N, Somani B, Rai B, Aboumarzouk OM. Treatment options for calyceal diverticula. Curr Urol Rep 2019; 20(7):37. doi: 10.1007/s11934-019-0900-x.
- Rapp DE, Gerber GS. Management of caliceal diverticula. J Endourol 2004; 18(9):805-10. doi: 10.1089/end. 2004.18. 805.
- Yang H, Yao X, Tang C, Shan Y, Weng G. Flexible uretero-renoscopy management of calyceal diverticular calculi. Urol J 2019; 16(1):12-15. doi: 10.22037/uj.v0i0.4002.
- Boonyapalanant C, Saksirisampant P, Taweemonkongsap T, Leewansangtong S, Srinualnad S, Chotikawanich E. Factors ımpacting stone-free rate after retrograde ıntrarenal surgery for calyceal diverticular calculi. Res Rep Urol 2020; 12:345-50. doi: 10.2147/RRU.S265959.
- Erkurt B, Kiremit MC, Altay B, Guzelburc V, Soytas M, Erdogan F, et al. Is retrograde flexible nephrolithotripsy feasible for calyceal diverticular stone? Urolithiasis 2014; 42(4):347-51. doi: 10.1007/s00240-014-0672-1.
- Monga M, Smith R, Ferral H, Thomas R. Percutaneous ablation of caliceal diverticulum: Long-term followup. J Urol 2000 Jan;163(1):28-32.
- Waingankar N, Hayek S, Smith AD, Okeke Z. Calyceal diverticula: A comprehensive review. Rev Urol 2014; 16(1):29-43.
- Mangin P, Mitre A, Pascal B, Cukier J. Les diverticules caliciels. Revue de 80 diverticules chez 70 patients [Calyceal diverticula : Review of 80 diverticula in 70 patients (author's transl)]. J Urol (Paris) 1980; 86(9):653-4. PMID: 6782168.
- Abeshouse BS, Abeshouse GA. Calyceal diverticulum: A report of sixteen cases and review of the literature. Urol Int 1963; 15:329-57. doi: 10.1159/000279027.
- Turna B, Raza A, Moussa S, Smith G, Tolley DA. Management of calyceal diverticular stones with extracorporeal shock wave lithotripsy and percutaneous nephrolithotomy: Long-term outcome. BJU Int 2007; 100(1):151-6. doi: 10.1111/j.1464-410X.2007.06911.x.
- Ito H, Aboumarzouk OM, Abushamma F, Keeley FX Jr. Systematic review of caliceal diverticulum. J Endourol 2018; 32(10):961-72. doi: 10.1089/end.2018.0332.
- Sabnis RB, Ganesamoni R, Doshi A, Ganpule AP, Jagtap J, Desai MR. Micropercutaneous nephrolithotomy (microperc) vs retrograde intrarenal surgery for the management of small renal calculi: A randomised controlled trial. BJU Int 2013 Aug;112(3):355-61. doi: 10.1111/bju.12164.
- Meng H, Chen S, Chen G, Tan F, Wang C, Shen B. Renal subcapsular hemorrhage complicating ureterolithotripsy: An unknown complication of a known day-to-day procedure. Urol Int 2013; 91(3):335-9. doi: 10.1159/000 350891.
- Tao W, Cai CJ, Sun CY, Xue BX, Shan YX. Subcapsular renal hematoma after ureteroscopy with holmium: Yttrium-aluminum-garnet laser lithotripsy. Lasers Med Sci 2015; 30(5):1527-32. doi: 10.1007/s10103-015-1760-3.
- Whitehurst LA, Somani BK. Perirenal Hematoma After Ureteroscopy: A systematic review. J Endourol 2017; 31(5):438-45. doi: 10.1089/end.2016.0832.
- Chong TW, Bui MH, Fuchs GJ. Calyceal diverticula: Ureteroscopic management. Urol Clin North Am 2000; 27(4):647-54. doi: 10.1016/s0094-0143(05)70114-2.