An Intriguing Case of Back Pain in an Elderly Male
By Muhammad Mohsin Sajjad1, Adnan Nasir2, Hamid Shahzad1Affiliations
doi: 10.29271/jcpsp.2022.12.1646Sir,
Breast cancer is a rare malignancy in men. Thus, it is often ignored and leads to delayed diagnosis and late presentation. It commonly metastasizes to bone, and axial skeleton is the preferred area of involvement. Low backache is a common symptom in all age groups and a leading cause of physical disability in the world. Worldwide, years spent with disability increased by 54% between 1990 and 2015, with the biggest increase seen in low-income and middle-income countries.1 It may rarely manifest as an initial presentation of malignancy. For the majority of presentations of back pain, the diagnosis is difficult and it has given rise to the term “non-specific low back pain,” which is generally managed at primary care and considered benign.2 Breast cancer should be considered in a list of differential diagnoses in patients presenting with back pain.
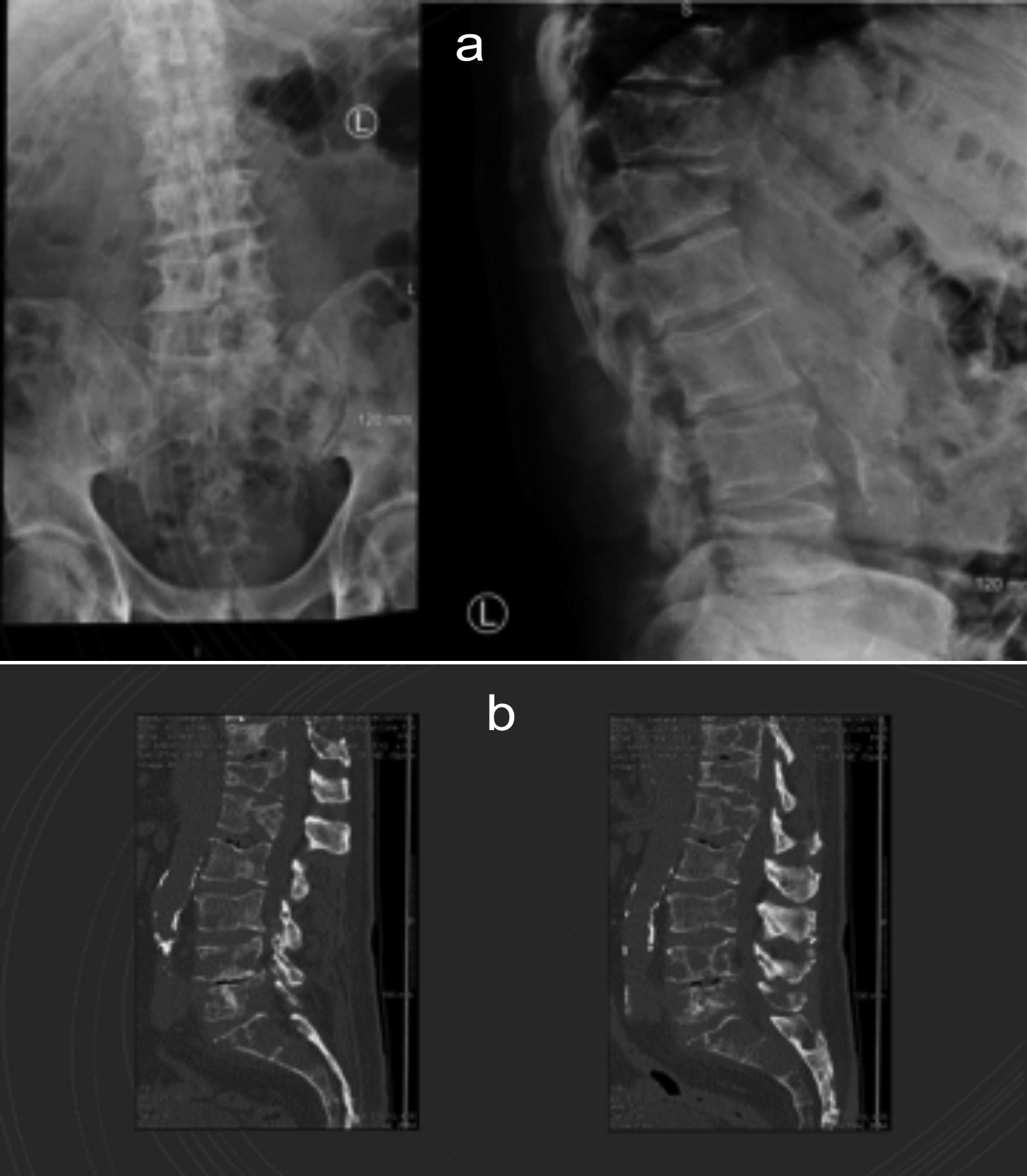 Figure 1: (A) X-ray lumbosacral spine (AP view) (B) Lateral view.
Figure 1: (A) X-ray lumbosacral spine (AP view) (B) Lateral view.
We report a case of 77-year man with a one-month history of intermittent severe left loin pain with recent extension into the left leg, mobilising only with severe pain. Background history was significant for hypertension, diabetes, dyslipidemia, and mild left ventricular hypertrophy. The back pain was progressively worsening for 5 to 6 weeks. Initially, it started as bilateral hip pain, migrated to the mid lower back, worsening with mobility with minimal weight loss. An X-ray was performed which showed lytic lesions and pathological fractures of T12 and L1 vertebrae (Figure 1). Screening for multiple myeloma was negative. A careful examination of the breasts revealed a 3×2 cm hard lump with irregular margins involving the left breast. CT-guided biopsy of the breast mass (Figure 2) revealed invasive ductal carcinoma.
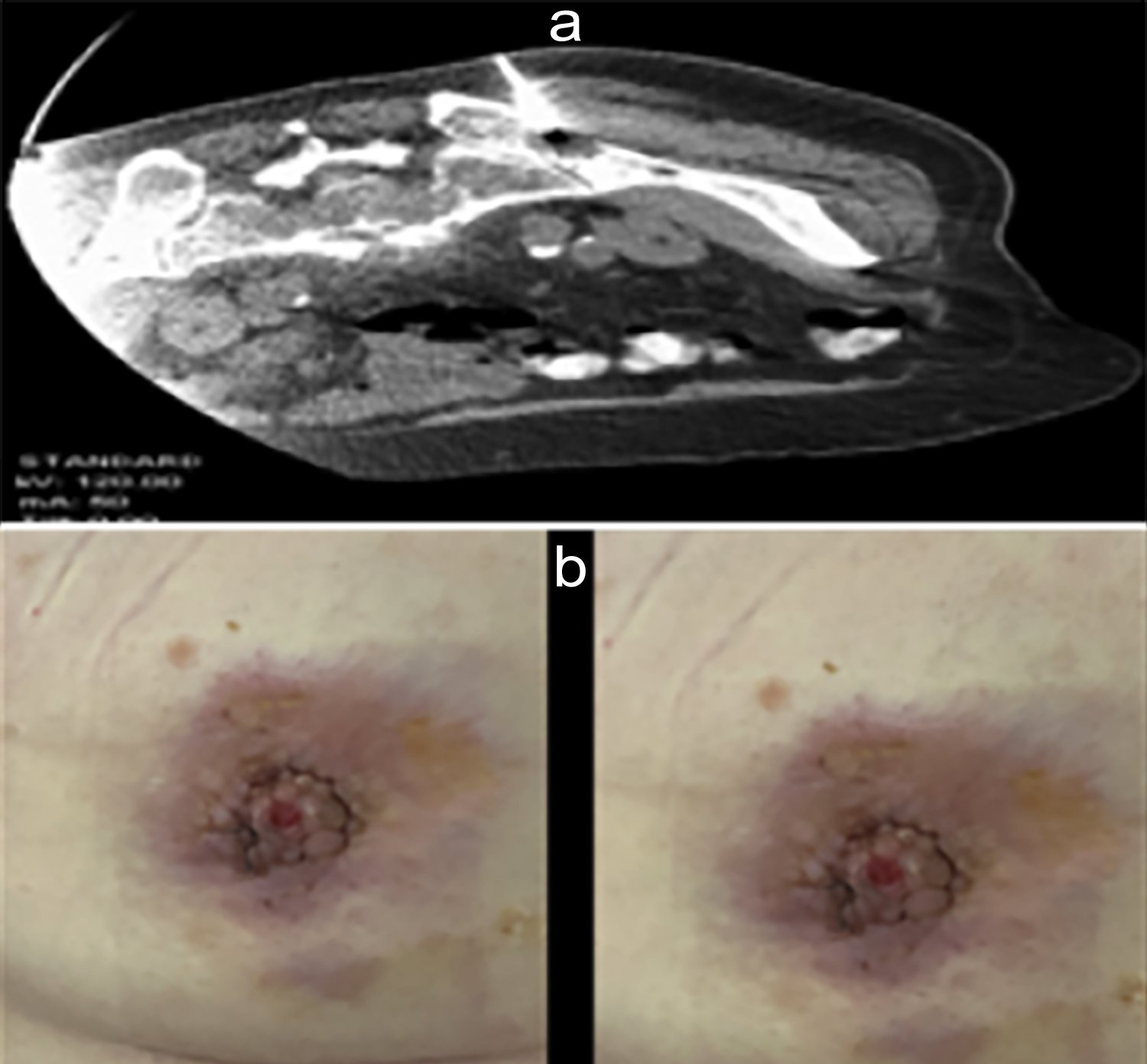 Figure 2: (A) CT-guided biopsy (B) Breast lump, 2 ×3 cm hard lump with irregular margins, retracted nipple, and blood-stained discharge.
Figure 2: (A) CT-guided biopsy (B) Breast lump, 2 ×3 cm hard lump with irregular margins, retracted nipple, and blood-stained discharge.
Backache can rarely be the initial presentation of malignancy. In patients presenting with low back pain to the primary care, spinal fracture constitutes 1 to 4%, and malignancy constitutes 1%, whether primary tumour or metastasis.3 Early detection of spinal malignancy is important as it can prevent the further spread of metastatic disease.4
Backache is a common symptom of presentation to the general practitioner. Metastatic disease should be kept in the list of differential diagnoses, especially in the elderly population or whenever there are red flag signs. Breast cancer, although rare in men, can present with low back pain. A careful physical examination can help in picking up early nodules, lumps and any abnormal discharge from the breast and can prevent late diagnosis and complications.
COMPETING INTEREST:
The authors declared no competing interest.
AUTHORS’ CONTRIBUTION:
MMS, AN, HS: Described and drafted the manuscript.
REFERENCES
- Hartvigsen J, Hancock MJ, Kongsted A, Louw Q, Ferreira ML, Genevay S, et al. What low back pain is and why we need to pay attention. Lancet 2018; 391(10137):2356-67. doi: 10.1016/S0140-6736(18)30480-X.
- Koes BW, Van Tulder M, Lin CW, Macedo LG, McAuley J, Maher C. An updated overview of clinical guidelines for the management of non-specific low back pain in primary care. European Spine J 2010; 19(12):2075-94. doi: 10.1007/ s00586-010-1502-y.
- Williams CM, Henschke N, Maher CG, van Tulder MW, Koes BW, Macaskill P, et al. Red flags to screen for vertebral fracture in patients presenting with low‐back pain. Cochrane Database Syst Rev 2013; (1):CD008643. doi: 10.1002/14651858.CD008643.pub2.
- Loblaw DA, Perry J, Chambers A, Laperriere NJ. Systematic review of the diagnosis and management of malignant extradural spinal cord compression: The cancer care ontario practice guidelines initiative’s neuro-oncology disease site group. J Clin Oncol 2005; 23(9):2028-37. doi: 10.1200/JCO.2005.00.067.