A Case of Unilateral Aplasia Cutis Congenita on the Hand in a Newborn Male Baby Exposed to Low Molecular Weight Heparin in Utero
By Dilek Mentesoglu1, Halil Kose2Affiliations
doi: 10.29271/jcpsp.2023.01.122Sir,
A 38-weeks male baby with a birth weight of 3400g was born by cesarean section. The newborn was consulted to dermatology due to absence of the skin on the hand. Apgar scores were 8 and 10 at 1 and 5 minutes, respectively. There was no history of aplasia cutis congenita (ACC) or any congenital anomalies. The mother was a 39-year healthy primigravid woman. Bemiparin, low molecular weight heparin, was the only drug taken during pregnancy to prevent early pregnancy loss. She denied exposure to teratogenic agents, radiation, alcohol, other drugs, intrauterine trauma, or infections during the pregnancy.
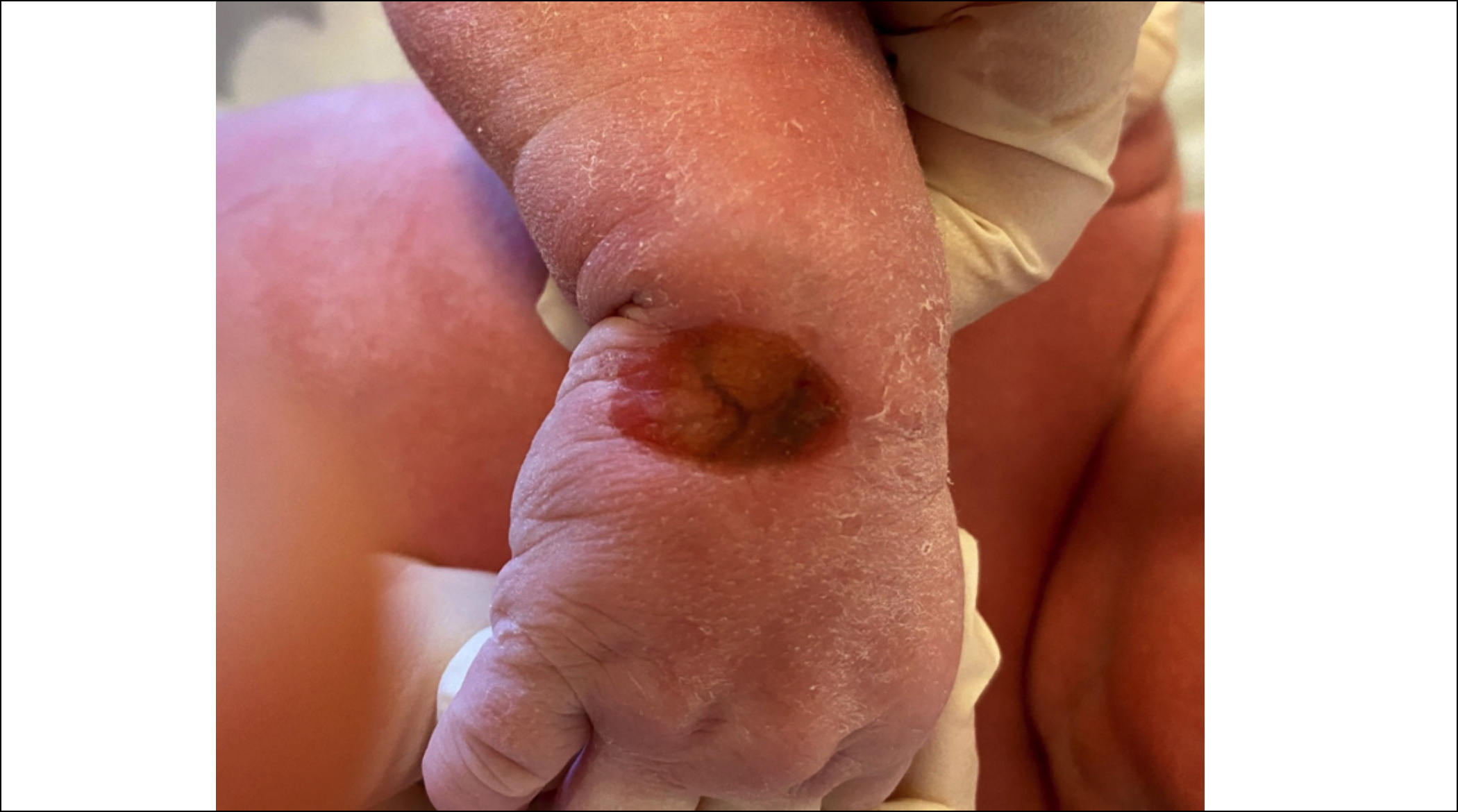 Figure 1A: Skin defect on the dorsum of the right hand at birth.
Figure 1A: Skin defect on the dorsum of the right hand at birth.
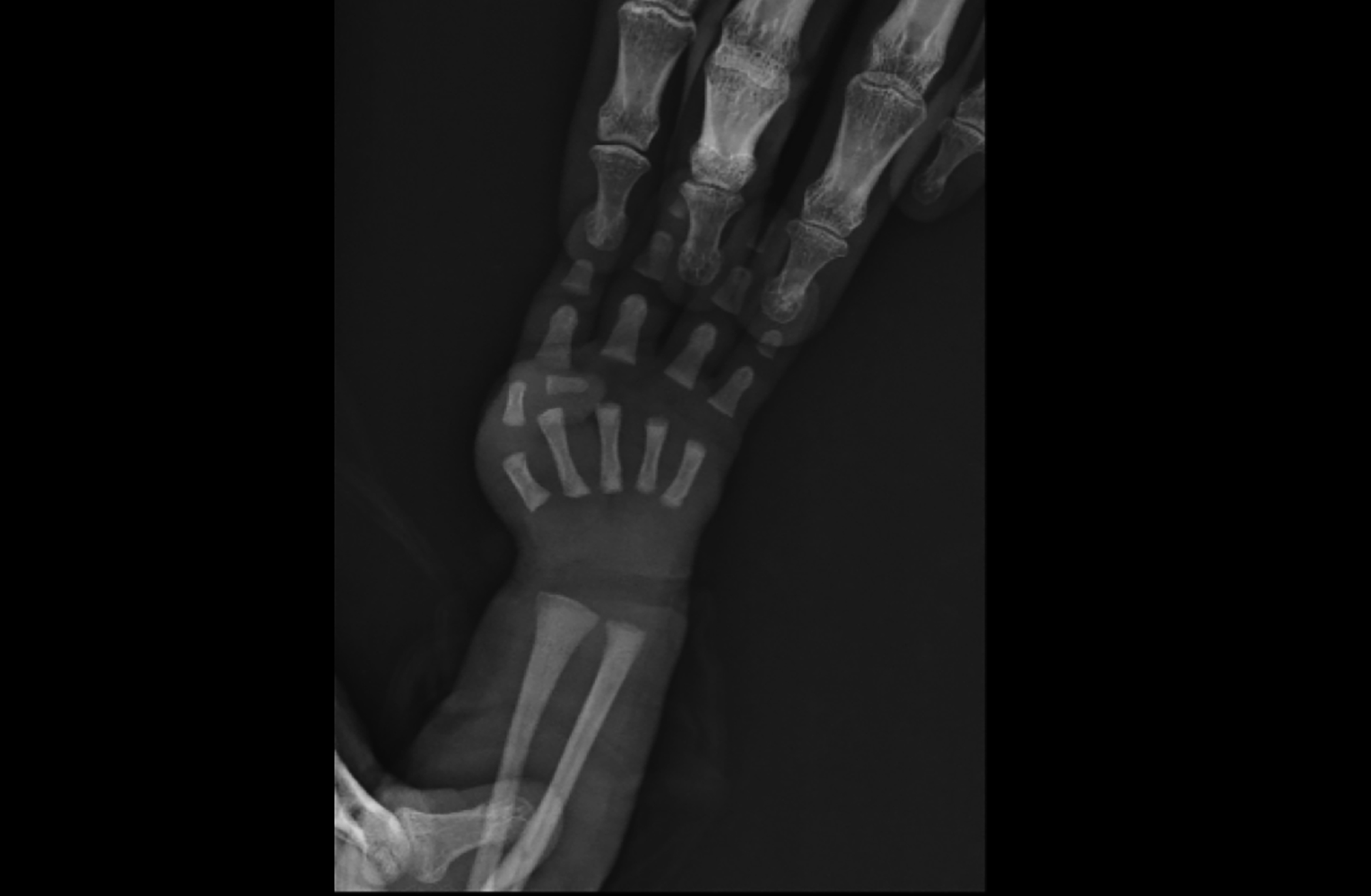 Figure 1B: The patient's hand X-ray appears normal.
Figure 1B: The patient's hand X-ray appears normal.
Dermatological examination revealed a well-defined ulcer with a total absence of skin measuring 2 cm x 3 cm on the dorsum of the right hand (Figure 1A). No lesions such as blistering or nail abnormality were detected elsewhere. A hand X-ray was performed to rule out possible bone anomalies; no defects were found (Figure 1B). Transfontanellar and an abdominal ultrasound scans and all metabolic and laboratory investigations were normal. Therefore, according to the classification outlined by Frieden,¹ we established the diagnosis of type VII ACC. Primarily, conservative therapy was adopted, comprising of attentive sanitary care, protection from environmental factors, and non-adhering dressings containing paraffin tulle coated with chlorhexidine twice a day. Wound healing progress was visible within two weeks (Figure 1C).
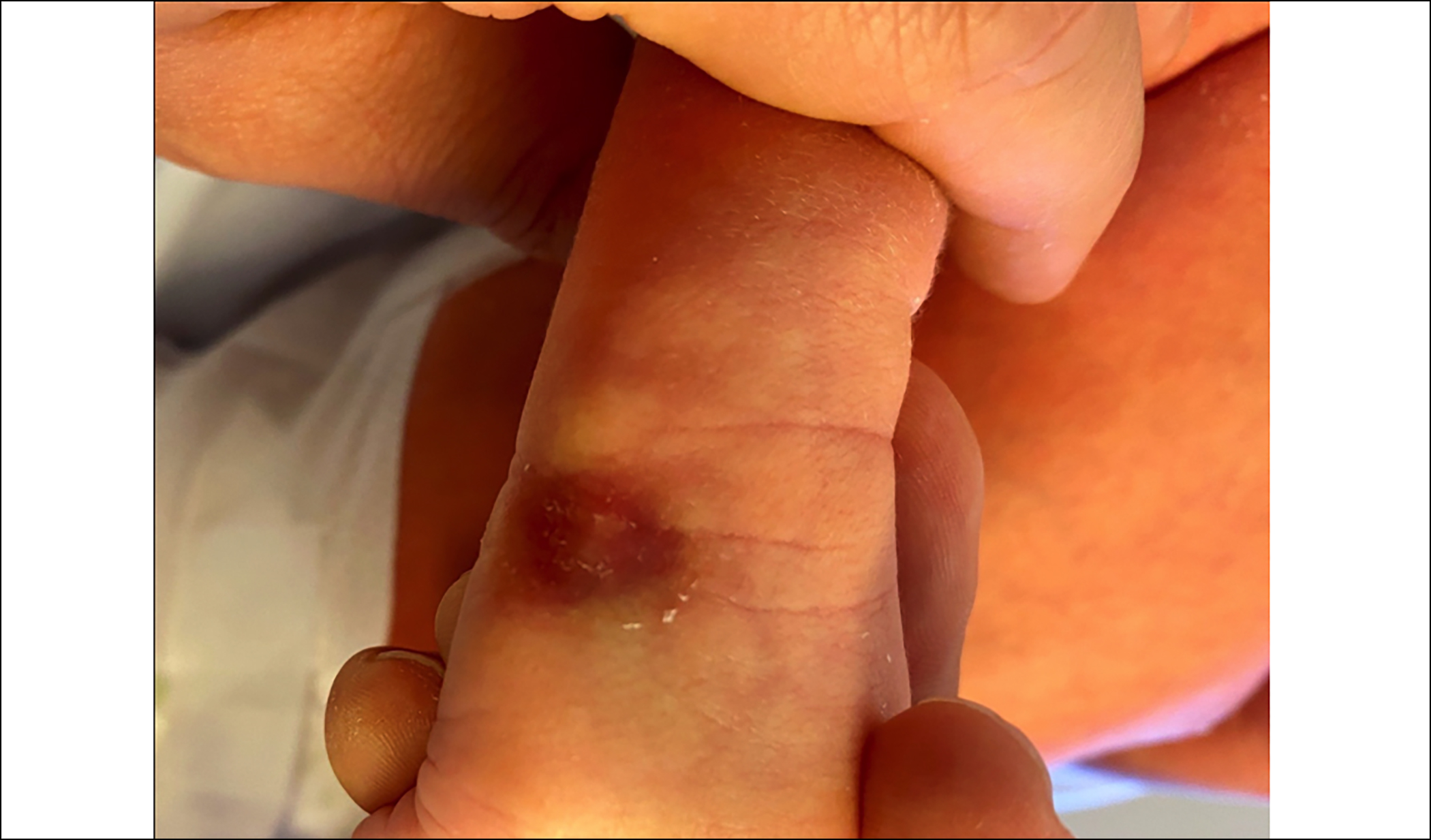 Figure 1C : Skin defect on the dorsum of the right hand on day 14 of life.
Figure 1C : Skin defect on the dorsum of the right hand on day 14 of life.
ACC is most commonly seen on the scalp.² In association with radial dysplasia, ACC in the upper extremities is known in the literature, but only small case series are reported because of the rarity. Davidson et al. reported four cases of radial dysplasia associated with ACC of the distal forearm. However, no skeletal anomaly was defined at birth in any patients.³ Therefore, although, no ipsilateral bone anomalies were detected at birth, this patient will be followed closely.
An isolated case of scalp ACC has been reported with a possible association with tinzaparin.⁴ However, the fact that aplasia cutis is a multifactorial disease with an unexplained cause in most instances, makes it difficult to establish a direct relationship with bemiparin. The newborns affected by ACC should be carefully examined to exclude concomitant possible congenital malformations and establish a suitable treatment. The detailed drug history of the pregnant woman should be questioned regarding teratogenic agents. Also, genetic counselling should be given to the family against the risk of recurrence in subsequent births.
COMPETING INTEREST:
The authors declared no competing interest.
AUTHORS’ CONTRIBUTION:
DM: Concept, visualization, data collection, literature search, and draft writing.
HK: Data collection, data analysis, and draft review.
All authors have confirmed the final version of the manuscript.
REFERENCES
- Frieden IJ. Aplasia cutis congenita: A clinical review and proposal for classification. J Am Acad Dermatol 1986; 14(4):646-60. doi: 10.1016/s0190-9622(86)70082-0.
- Oliveira RS, Juca CEB, Lins-Neto AL, Rego MAC, Farina J, Machado HR. Aplasia cutis congênita of the scalp: Is there a better strategy? Childs Nerv Syst 2006; 22(9):1072-9. doi: 10.1007/s00381-006-0074-y.
- Davidson AW, Hosalkar HS, Hill RA, Monsell F. Radial dysplasia with localised cutis aplasia congenita. J Pediatr Orthop B 2003 ; 12(6):398-401. doi: 10.1097/01.bpb. 0000060283.77027.5f.
- Sharif S, Hay CRM, Clayton-Smith J. Aplasia cutis congenita and low molecular weight heparin. BJOG 2005; 112(2): 256-8. doi: 10.1111/j.1471-0528.2004.00347.x.